18 Sep 2020 What You Need to Know About Health Savings Accounts
The Health Savings Account (HSA) is one of the most misunderstood and underused benefits in the Internal Revenue Code. Congress created HSAs as a way for individuals with high-deductible health plans (HDHPs) to save for medical expenses that are not covered by insurance due to the high-deductible provisions of their insurance coverage.
HSA as a Retirement Vehicle
Although the tax code refers to these plans as “health” savings accounts, an HSA can act as more than just a vehicle to pay medical expenses; it can also serve as a retirement account. For some taxpayers who have maxed out their retirement plan options, an HSA provides another resource for retirement savings—one that isn’t limited by income restrictions in the way that IRA contributions are.
Since there is no requirement that the funds be used to pay medical expenses, a taxpayer can pay medical expenses with other funds, allowing the HSA to grow (through account earnings and further tax-deductible contributions) until retirement. In addition, should the need arise, the taxpayer can still take tax-free distributions from the HSA to pay medical expenses. Unlike traditional IRAs, no minimum distributions are required from HSAs at any specific age.
Withdrawals from an HSA that aren’t used for medical expenses are taxable and subject to a 20% penalty, with one exception: an individual age 65 or older will pay income tax on non-medical related distributions from their HSA but won’t owe a penalty for using the funds for other than medical expenses.
Example: Henry, age 70, has an HSA account from which he withdraws $10,000 during the year. He also has unreimbursed medical expenses of $4,000. Of his $10,000 withdrawal, $6,000 ($10,000 – $4,000) is added to Henry’s income for the year, and the other $4,000 is both tax- and penalty-free. If Henry had been 64 years old or younger, he’d be taxed on the $6,000 and pay a penalty of $1,200 (20% of $6,000).
Eligible Individual – To be eligible to contribute to an HSA in a given month, an individual:
1. must be covered under an HDHP on the first day of the month;
2. must NOT also be covered by any other health plan (although there are some exceptions);
3. must NOT be entitled to Medicare benefits (i.e., generally must be younger than age 65); and
4. must NOT be claimed as a dependent on someone else’s return.
Any eligible individual—whether employed, unemployed or self-employed—can contribute to an HSA. Unlike with an IRA, there is no requirement that the individual have compensation, and there are no phase-out rules for high-income taxpayers. If an HSA is established by an employer, then the employee and/or the employer can contribute. Not just family members but any other person can make contributions to HSAs on behalf of eligible individuals. Both employer contributions and employee contributions made via the employer’s cafeteria plan are excluded from the employee’s gross income. Employees who make HSA contributions outside of their employers’ arrangements are eligible to take above-the-line deductions—that is, they don’t need to itemize deductions—for those contributions.
The Monetary Qualifications for an HDHP: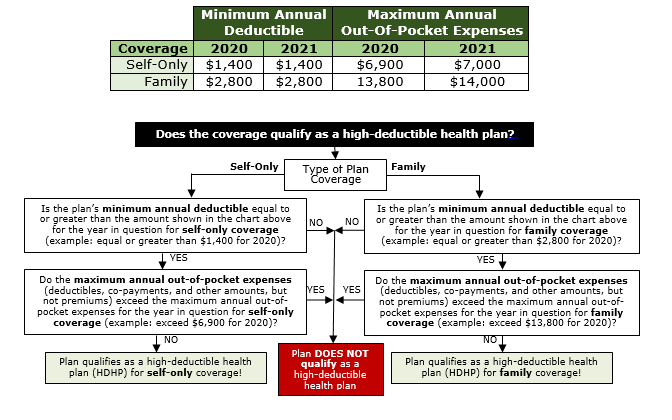
Example—Family Plan Does Not Qualify: Joe has purchased a medical insurance plan for himself and his family. The plan pays the covered medical expenses of any member of Joe’s family if that family member has incurred covered medical expenses of over $1,000 during the year, even if the family as a whole has not incurred medical expenses of over $2,800 during that year. Thus, if Joe’s medical expenses are $1,500 during the year, the plan would pay $500. This plan does not qualify as an HDHP because it provides family coverage with an annual deductible of less than $2,800.
Example—Family Plan Qualifies: If the coverage for Joe and his family from the example above included a $5,000 family deductible and provided payments for covered medical expenses only if any member of Joe’s family incurred over $2,800 of expenses, the plan would then qualify as an HDHP.
Maximum Contribution Amounts – The amounts that can be contributed are determined on a monthly basis and are calculated by dividing the annual amounts shown below by 12. Thus, if an individual’s health plan only qualified that person for an HSA for 6 months out of the year, then that person’s contribution amount would be half of the amount shown.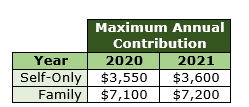
In addition to the amounts shown, an eligible individual who is age 55 or older can contribute an additional $1,000 per year.
How HSAs are Established – An eligible individual can establish one or more HSAs via a qualified HSA trustee or custodian (an insurance company, bank, or similar financial institution) in much the same way that an individual would establish an IRA. No permission or authorization from the IRS is required. The individual also is not required to have earned income. If employed, any eligible individual can establish an HSA with or without the employer’s involvement. Joint HSAs between a husband and wife are not allowed, however; each spouse must have a separate HSA (and only if eligible).
Qualified Medical Expenses – To be non-taxable and penalty-free, distributions must be for unreimbursed expenses paid by the HSA account owner, their spouse, or dependents for medical expenses that have the same definition as medical expenses for purposes of the medical itemized deduction.
Amounts paid for medicine or drugs are qualified medical expenses for HSA distribution purposes only if the medicine or drug is prescribed (determined without regard to whether such a drug is available without a prescription) or insulin.
The qualified medical expenses must be incurred only after the HSA has been established, and medical expenses paid or reimbursed by HSA distributions cannot also be claimed as medical expenses for itemized deduction purposes.
Generally, health insurance premiums are NOT qualified medical expenses for HSA purposes, except for the following:
- Qualified long-term care insurance (but only up to the amount of the annual age-based limit that applies for deducting long-term care premiums as medical expenses);
- COBRA health care continuation coverage;
- Health care coverage while receiving unemployment compensation; and
- For individuals age 65 or over, premiums for Medicare A, B, or D, Medicare HMO, and the employee share of premiums for employer-sponsored health insurance, including premiums for employer-sponsored retiree health insurance (but not Medigap policies).
Menstrual Products – Effective for tax years 2020 and later, the CARES Act added a provision that permits tax-free reimbursement from health savings accounts for costs of menstrual products.
Telehealth – The rule has been that taxpayers may only make contributions to HSAs while they are covered by a high-deductible health plan. However, the CARES Act allows a high-deductible health plan to provide telehealth and remote care services without a deductible for 2020 and 2021.
If you have questions related to the medical tax benefits of an HSA or how an HSA can supplement your retirement planning, please Contact Us.

